Featured Items

The Fight Against Pneumonia-Induced Child Mortality. A Case Study from Mozambique.

Joan Tubau*
last updated: 10 November 2020
EDITORS’ NOTE: This text was written in early 2020, when the COVID-19 epidemic had not yet become a global health emergency. Since then, like other nations, Mozambique has had to address the economic, social and health challenge of the coronavirus, including its collateral effects on other health priorities. Although Mozambique’s official COVID-19 figures seem modest compared to those of the hardest-hit countries—13,577 cases and 99 deaths confirmed by World Health Organisation, according to the most recent reports—the true magnitude of the epidemic may, in fact, be greater. More importantly, COVID-19 has taken an indirect toll by hindering the response to the country’s main causes of morbidity and mortality. Childhood vaccination programmes against pneumonia are among the most dramatic examples.
Since it is currently impossible to reassess the situation on the ground, we have chosen to commemorate World Pneumonia Day by publishing the text as it was originally written, updating the statistical information wherever possible. Readers should note that COVID-19 has only exacerbated and complicated the harsh reality described below.

Paediatric care at the Manhiça hospital, in Mozambique. (ISGlobal)
1. Félix Sande’s Paediatric Practice
It’s 9:00 a.m. and Félix Sande has already been seeing patients at the Manchiana Health Unit for over an hour. Félix is an agente de medicina general, or general medicine agent—a difficult-to-categorise type of health professional who, as in most of Mozambique’s outlying health care facilities, holds the lives of local children in his hands.
Félix knows the people of the surrounding area well. Although he was born in central Mozambique, for more than nine years he has worked at this small health centre, where on countless occasions he has confronted the ancient enemies of the children he serves. It’s early December, the start of the summer in the southern hemisphere. Nevertheless, it’s rainy and cold—and that is not a good thing.
“We are in the peak season,” Félix explains. “Malaria is on the rise, accounting for 45% to 50% of the patients I see on any given day. Respiratory infections are also rising. Although the situation is better than it was a few years ago, I am still seeing many children with pneumonia.”
In the health centre’s waiting area, nearly two dozen women take shelter from the light rain, clutching their children in their arms. They have walked for over an hour to seek paediatric care for their children. Despite their long trek in the rainy and unexpectedly cold weather, despite having to leave other small children at home with a sister or a neighbour, and despite having missed out on a whole day’s work in the machamba, they are happy. They are unusually fortunate, and they know it.
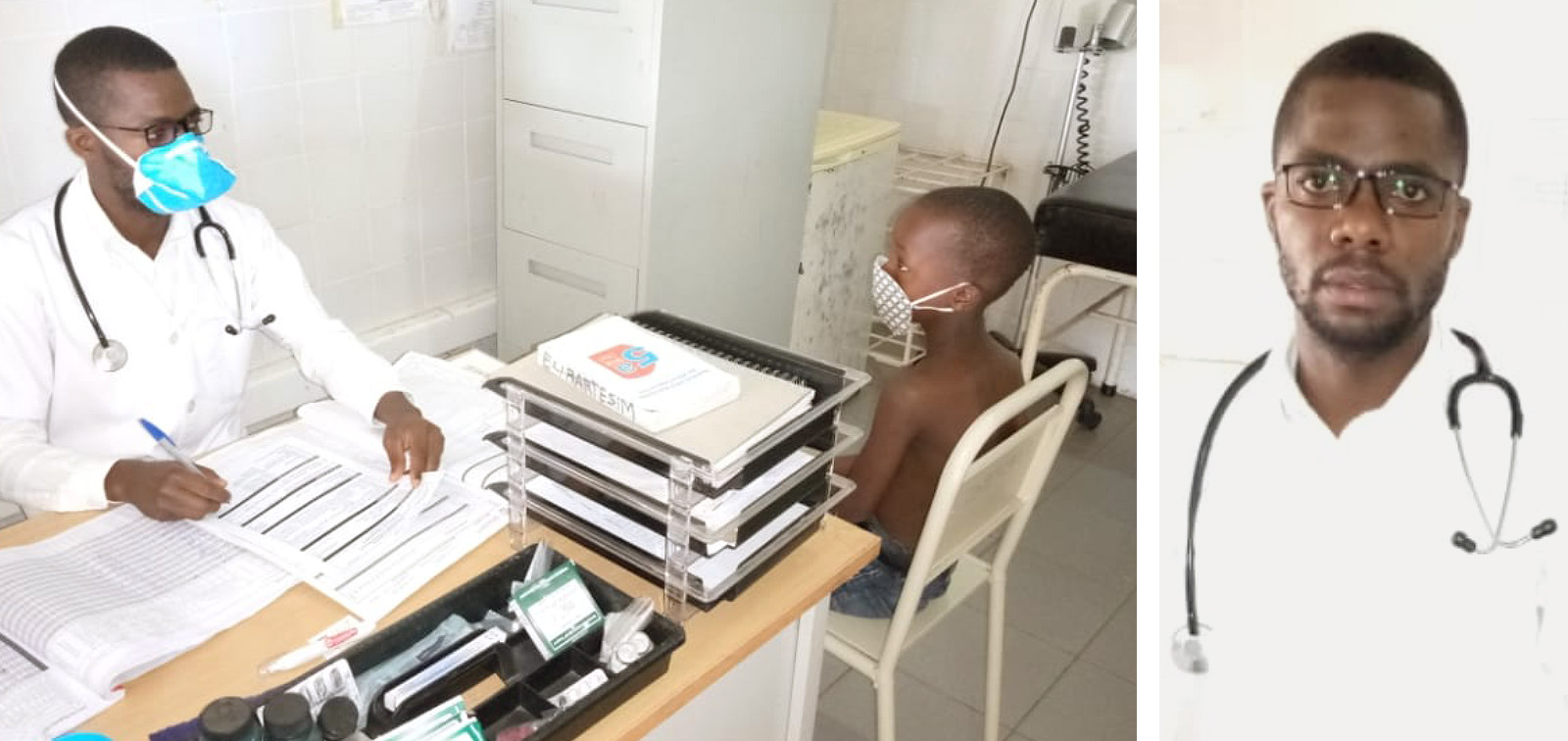
Félix Sande sees a patient at the Manchiana Health Unit, in Mozambique. (CISM)
At his paediatric practice in Manchiana, Félix attends to the children empathetically, not only diagnosing their ailments but also carrying out full health assessments. “Vaccination coverage is high in our district,” he explains. “When I see children who are missing a dose, I refer them to the health unit’s nurse, who provides a catch-up dose. I do the same whenever I encounter an acutely malnourished child. The nurse has ready-to-use therapeutic food on hand and is able to provide the necessary treatment for the child to take at home.”
Félix’s well-organised office is stocked with the basic medicines required for treating the most common diseases affecting children in Mozambique. He is trained to detect when a child requires care that he cannot provide and must be referred to Manhiça Hospital, which is about 15 kilometres away.
Last month, Félix treated 573 children at his paediatric practice. Three required immediate hospitalisation: two with malaria and one with pneumonia.
The Manchiana Health Unit and its paediatric practice—like the wider health system of Manhiça District, in southern Mozambique—are simultaneously an extraordinary experience and a terrible exception
A Land Cruiser from Manhiça Hospital, which serves as an ambulance when necessary, picked up the three children and their mothers and transported them to the hospital.
This operation was carried out quickly and at no cost to the families of the three gravely ill children. All three recovered quickly after receiving the care they needed at the hospital.
While this might seem normal in cases of severe illness in young children, is not common in Mozambique. In fact, in most cases it is mortally inconceivable.
The Manchiana Health Unit and its paediatric practice—like the wider health system of Manhiça District, in southern Mozambique—are simultaneously an extraordinary experience and a terrible exception. Both owe their existence to the Manhiça Health Research Centre (CISM).

CISM main entrance, in Mozambique. (ISGlobal)
More than 20 years ago, a group of Spanish doctors founded a health care and research centre in Manhiça that eventually became CISM. This group of physicians and researchers, led by Dr. Pedro Alonso, had a very simple objective: to put medical research and scientific evidence at the service of the people of Mozambique who were dying prematurely from easily preventable and curable diseases.
Over the years, thanks to the efforts of numerous people and institutions—notably the Spanish Agency for International Development Cooperation—CISM has emerged as an extraordinary example of experience-based medicine at the service of the population. The medical research promoted by these backers—which is largely carried out by African doctors trained at the centre—has generated, among much else, the evidence needed to definitively push for pneumococcal conjugate vaccines (PCV10 and PCV13) to be included in Mozambique’s Expanded Programme on Immunisation, which is largely responsible for the radical decrease in the country’s incidence of pneumonia.
The presence of CISM and the empowerment it brought to Manhiça’s health system also explain why the district’s 180,000 people have significantly better health care access than the rest of the country. This access, in turn, has fuelled a sharp reduction in the district’s under-five mortality rate, which is now half that of the country as a whole.
As we took leave of Félix, his last words conveyed understandable pride and, at the same time, heartbreaking sorrow: “If everyone in Mozambique had the same health care as Manhiça, our country would be a different place and the future of our people would be radically better and fairer.”
2. The Injustice of Thousands of Preventable Deaths
Robust statistics about the health status of Mozambique’s under-five population are hard to come by.
Even so, the available figures endorsed by the Ministry of Health and the United Nations agencies and organisations operating in the country paint a heartbreaking picture of the health and lives of the vast majority of Mozambicans.
In 2019, 54 of every thousand children born alive in Mozambique died before their first birthday. This is three times the rate of preventable deaths set as a target for the year 2030 by the Sustainable Development Goals (SDGs). These children die from infectious diseases that are easy and cheap to prevent and cure; 35% of them die from malaria, and the rest from diarrhoea and acute respiratory infections, particularly pneumonia.
Before reaching their fifth birthday, 72 out of every thousand children sadly lose their lives at the hands of the usual enemies; this rate, too, is three times the SDG target set for 2030.
The most recent retrospective mortality survey carried out in Mozambique found that deaths among children under one year of age accounted for 25% of all deaths over the course of a year. (By way of contrast, in Spain fewer than 1 in 100 people die before reaching 20 years of age.) Less than 50% of these doomed children received any sort of medical care or clinical treatment during their illness—the lowest percentage for any age group in Mozambique and an indication of the staggering vulnerability of the country’s children.
Pneumonia is a preventable disease that is relatively easy to diagnose and treat, yet it accounts for nearly 13% of deaths in children under five years of age each year. Ten out of every thousand children born alive in Mozambique in a given year will die of pneumonia; this rate is three times the target set by the Global Action Plan for Pneumonia and Diarrhoea (GAPPD) for just five years from now. This loss of life is absolutely unacceptable, given that nowadays pneumonia is a disease that is almost completely prevented by the vaccines included in the Expanded Programme on Immunisation. It is also a disease that can easily be diagnosed clinically by a community health worker with basic training and treated with amoxicillin, a very inexpensive antibiotic discovered nearly 50 years ago, which in Mozambique has proven very effective in all patients.
However, the most critical accomplices to pneumonia’s ongoing—and inexplicable—slaughter of children in Mozambique may be the country’s high rates of chronic malnutrition and HIV infection.
In Mozambique, approximately 43% of all children under five years of age are chronically malnourished; in some provinces in the north of the country, this rate rises to upwards of 50%. These are children who before two years of age do not receive a suitable diet rich in the nutrients necessary to guarantee health and proper development; in many cases, moreover, they are not exclusively breastfed for the first six months of life.
Mozambique is among the countries of southern Africa hit the hardest by the HIV pandemic. The HIV prevalence rate is approximately 12.6% nationwide and as high as 24% in some provinces.
Approximately one in four women who become pregnant in Mozambique are HIV-positive.
Bacterial pneumonia is the most common opportunistic infection among people living with HIV in Mozambique
Although great progress has been made thanks to multi-sector efforts, only around 50% of people in need of antiretroviral treatment in Mozambique receive it.
It is clear that HIV has a devastating direct effect on the immune system of people who do not receive adequate treatment and is a critical risk factor for opportunistic infections. Bacterial pneumonia is the most common opportunistic infection among people living with HIV in Mozambique, including children under five years of age.It is probably also the most deadly.
3. Poverty, Inequality and an Under-resourced System
It is useless to look for a single cause behind Mozambique’s current health outlook that would explain why, despite multiple initiatives and undeniable progress, the situation for the vast majority of the country’s people is far from fair and dignified.
Even so, it is clear that certain socioeconomic realities have a radical impact on people’s health and well-being, as well as on the country’s macroeconomic indicators, which currently paint a bleak picture.
Years of general economic growth in Mozambique have not translated into a noticeable impact on people’s daily lives and ability to meet their basic needs in a decent manner.
In 2019, 60% of Mozambique’s population was still living on less than €1 a day.
As a consequence of a debt crisis caused by opacity and highly dubious legal management on the part of the government, the country’s GDP has fallen and prices have risen across the board; the price of staple foods, in particular, has increased by more than 40%.
Logically, this situation has had a catastrophic impact on the nutritional situation of the country as a whole and of children under five years of age in particular.
Despite the fact that basic health services have virtually no direct cost for the population, structural poverty is a radical determinant of the strategic decisions made by families—and mothers in particular—who must weigh the inevitable opportunity costs associated with turning to the health system in the event of illness. The decision to take part in preventive programmes is, if anything, even more difficult.
Despite being widespread, poverty in Mozambique is undeniably unequal. The central and northern provinces—strongholds of the opposition party dating back to the civil war—have significantly worse economic, social and health indicators than the southern provinces and the capital city.
Ninety percent of Mozambique’s population lives more than one hour’s walk from the nearest health unit or clinic
But Mozambique is also characterised by vast inequalities between men and women, ranking 138th out of 155 countries in gender equality. Just a fraction of the country’s women have access to secondary education and only one in four have the opportunity to complete their studies.
Mozambique’s preterm birth rate of 16.5%—the fifth highest in the world—is a direct cause of mortality in the first days and weeks of life. In many cases, preterm birth is a direct consequence of teenage pregnancy: 40% of first pregnancies occur in adolescents under 20 years of age. Young women who give birth for the first time before age 20 are four times more likely to die during childbirth than women who have their first child after that age. This reality adds up to a sobering fact: Mozambique’s maternal mortality rate is around 489 deaths per 100,000 births, an appalling 700% higher than the SDG target set for just 10 years from now.
In addition to poverty and inequality, the other major structural determinant of the country’s health situation is the fragility of the public health system and its inability to reach the population in a real, equitable and effective way.
Ninety percent of Mozambique’s population lives more than one hour’s walk from the nearest health unit or clinic, while another 40% lives more than 30 kilometres away.
In a country with approximately eight doctors per 100,000 inhabitants (compared with Spain’s rate of 395 doctors per 100,000 inhabitants), clinics are usually staffed by personnel who, despite their commitment, find it very difficult to provide their patients with quality diagnosis and treatment due to poor training and constant shortages of basic supplies and medicines, including those used to treat the most prevalent and deadly diseases.
When clinic staff encounter complicated cases, their ability to react is basically non-existent, since there is no system in place for referring patients to higher levels of care. Families in rural communities can do nothing but take their loved ones back home and watch them die.
Given this absence and inefficacy on the part of the health care system, particularly at the primary level, much of the population only turns to the formal system in extreme cases—quite often when it is already too late.
4. Successes and Setbacks
Despite the gulf between reality and the SDG targets—particularly the health-related indicators for Goal 3—very substantial progress has been made in the fight against pneumonia in recent years, thanks to the collective efforts of governments, national and multilateral donors, the scientific community, health professionals and Mozambican civil society.
Sustained investment in effective strategies—especially on preventing, diagnosing and treating pneumonia and controlling some of its main underlying determinants—is responsible for the largely encouraging trajectory of the fight against the disease and the suffering it causes.
In 1990, under-five mortality in Mozambique was 240 children per 1,000 live births. By 2018, this rate had fallen by over 70%, to 71 children per thousand live births.
Since 2000, mortality from pneumonia in Mozambique has decreased at a rate of 4.5% per year. Although precise figures are difficult to come by, it is clear that the fight against pneumonia in recent years has gone a long way towards preventing an outrageously large loss of life—both present and future—in Mozambique.
The great turning point in the fight against pneumonia in Mozambique was the inclusion of pneumococcal conjugate vaccines in the country’s Expanded Programme on Immunisation.
The introduction of 10-valent pneumococcal conjugate vaccine (PCV10) in 2013, followed by the 13-valent formulation (PCV13) in 2017, had a key impact on reducing pneumonia morbidity and mortality by ensuring that the disease was prevented very effectively in all properly vaccinated children.
Since then, thanks to the coordinated efforts of the Ministry of Health in collaboration with UNICEF—and, crucially, stable and predictable funding from Gavi, the Vaccine Alliance—PCV vaccines have been successfully incorporated into both the routine immunisation schedule and vaccination campaigns throughout the country. In Mozambican children, the rate of complete PCV coverage in the first year of life now stands at around 70%.
The coverage provided through the Expanded Programme on Immunisation does more than guarantee direct protection against pneumonia via PCV. With the introduction of the rotavirus vaccine and, in 2009, the Haemophilus influenzae type B (Hib) vaccine, children are also guaranteed protection against diarrhoea and meningitis in their first year of life. In addition to being terrible enemies in themselves, these ailments also dramatically increase a child’s chances of contracting and dying of pneumonia.
The other major strategy that has had a positive impact on the fight against pneumonia in recent years has been the expansion of early diagnosis and treatment—in other words, bringing diagnosis and treatment as close as possible to communities and patients.
The development and adoption of a clinical diagnostic protocol adapted to the capacities of the personnel working in Mozambique’s health units, the provision of stopwatches for measuring patients’ respiratory rate, the adoption of a protocol for treating pneumonia with dispersible amoxicillin tablets, and the availability of said tablets in the pharmacies of clinics in remote areas have made it possible for tens of thousands of children to receive an early and accurate pneumonia diagnosis.
The effectiveness of this strategy received an extraordinary boost when the Ministry of Health reintroduced the figure of the community health worker in 2010. After approximately four months of training, these workers—known in Mozambique as agentes polivalentes elementares (APEs)—are equipped not only to promote preventive measures but also to diagnose and treat the most common—and most deadly—diseases found in children under five years of age. As a part of this strategy, the Ministry of Health and its main partners—notably, the international organisation Save the Children—have created a nationwide network of approximately 5,300 APEs. These workers are capable of diagnosing pneumonia as soon as the first signs of illness appear and providing appropriate treatment with amoxicillin to prevent the disease from worsening and eventually killing the patient.
Without a doubt, the decentralisation of pneumonia diagnosis and treatment to the local level through the deployment of this network of community health workers has, along with the expansion of vaccination coverage, been a key winning strategy for combatting pneumonia. In a country where the formal health system has great difficulty reaching the majority of the population, any strategy that does not consider and overcome the hurdles to access cannot have a real positive impact on people’s lives and health.
Not all of the strategies that are essential to achieving the objectives of the fight against pneumonia have had the same transformative effect.
In 2019, the number of children who died of pneumonia in Mozambique was three times higher than the GAPPD target set for 2025.
Even given the complexity and multiplicity of factors in this battle, it is clear that basic investments in the three areas that are essential to the fight against pneumonia—protection, prevention, and diagnosis and treatment—has been uneven, insufficient and generally ineffective at putting us on the right track to achieve our vital goals.
43% of children under 5 years of age are chronically malnourished and in some northern provinces of the country this rate shoots up to over 50%
In Mozambique, indicators of chronic malnutrition and exclusive breastfeeding in the first six months of life are among the worst in the region and in the world.
Only 41% of Mozambican children are exclusively breastfed for the first six months of their lives, compared with nearly 60% in the wider region. Despite the evidence that breastfeeding is a critical protective factor for children’s present and future health, none of the strategies and efforts deployed to date have had a substantial impact on the beliefs and practices of most mothers in Mozambique. As a result, these indicators have worsened slightly over the past decade. The low rate of breastfeeding in Mozambique not only translates into low protection in the critical first months of life but also sets in motion a perverse cycle of malnutrition.
Chronic malnutrition is an underlying determinant of approximately 33% of mortality in children under 5 years of age.
In Mozambique, 43% of children under 5 years of age are chronically malnourished and in some northern provinces of the country this rate shoots up to over 50%.

Medical care in the Premature Unit of the Manhiça hospital, in Mozambique. (ISGlobal)
While progress has been made in the diagnosis and treatment of acute malnutrition, rates of chronic malnutrition in Mozambique have held steady for years. None of the strategies implemented to date have had a perceptible—let alone decisive—effect on the complex and diverse range of factors that lead to chronic malnutrition in children under five years of age.
Access to safe drinking water and basic sanitation is clearly essential to the prevention of pneumonia and other ailments—particularly diarrhoea—that weaken children’s general health and increase the likelihood of complications leading to death.
Mozambique’s overall indicators remain, incomprehensibly, deplorable.
Eleven percent of Mozambicans use surface water for drinking, cooking and personal hygiene—a larger percentage of the population than those who have access to running water, who make up just 9% of the population. Only 21% of the population has access to a basic sanitation network, and nearly 40% of people have no toilet or latrine at home and must therefore practice open defecation.
This is without doubt the biggest failure in the fight against pneumonia in Mozambique. It may also be the most critical health risk factor for the country’s children, and one that could jeopardise the pursuit of many of the SDGs in Mozambique for many decades to come.
Only 21% of the population has access to a basic sanitation network, and nearly 40% of people have no toilet or latrine at home
Finally, and despite the fact that the diagnosis and treatment of pneumonia—together with the expansion of vaccination coverage and the addition of the PCV vaccines—have been the key differential factor in the major advances of recent years, this strategy faces an extraordinary limiting factor: the weakness of the public health system. This weakness will make it very difficult to continue expanding early diagnosis and treatment effectively to all communities.
Approximately 30% of Mozambique’s population has access to health services of acceptable quality. To be sure, this percentage obscures the reality of unequal access favouring the southern provinces and Maputo.
Despite investments by the government and its partners, as well as financial contributions from both national and multilateral donors, the country’s network of health infrastructure remains sorely insufficient and inadequate, especially in rural areas.
The system also suffers from structural problems due to the lack of sustainable funding, the tremendous scarcity of well-trained professionals, constant shortages of basic supplies and medicines, and the practical absence of a functional patient referral system.
In the face of this reality, remarkable efforts have been made to provide care in the most remote communities via mobile strategies and campaigns. Even so, it is estimated that less than half of the children suspected of having contracted pneumonia in Mozambique are currently receiving health care and proper diagnosis and treatment, which will undoubtedly lead to the cruellest of consequences: illness and death.

A group of workers of the CISM Social Sciences and Health Economics Unit has traveled to a rural area to carry out periodic supervision. (ISGlobal)
5. A Global Call to Action
Although many of the SDG targets set for 2030 seem out of reach today, we must remember that these targets constitute a collective international commitment and therefore represent an absolutely inescapable responsibility.
Looking ahead, it is essential to transform the current dynamic and chart a firm course that can save the lives of thousands of children. We must meet this challenge as an unwavering ambition: for humanity, for political accountability and perhaps as the last chance for an international system with little credibility left.
A decisive response is needed to address the major determinants of pneumonia and reduce mortality caused by this disease to the SDG target levels.
For such a transformation to be possible, all national and multi-sector stakeholders must redouble their efforts and commitments, particularly those with the greatest responsibilities, the most resources at their disposal and specific mandates to fulfil.
Forceful action is needed on those strategies most likely to yield effective results in the relatively short term in areas that are fundamental to controlling pneumonia and offer clear a return on investment.
A decisive response is needed to address the major determinants of pneumonia and reduce mortality caused by this disease to the SDG target levels
The government of Mozambique—and Mozambican society generally—are the parties with the greatest interest in building a future of justice and well-being for the country’s people. This is their responsibility and, indeed, their desire. Despite the country’s general difficulties, particularly its economic woes, this is a moment of opportunity. Mozambique has a new government that enjoys substantial political backing and has the political capital to promote transformative policies.
Even so, it is impossible to imagine that the Mozambican government could, in the next five or six years, accelerate and expand the strategies and actions needed to win the fight against pneumonia by 2030 while relying solely on its own resources.
Annual per capita health expenditure in Mozambique is approximately $40, which is 50% lower than the level recommended by the World Health Organisation and by a third of the African average. Unfortunately, these figures reflect the precarious financial situation of Mozambique’s health system.
Even in its shaky financial state, the system remains entirely dependent on external funding. Therefore, any reduction in funding has a real impact on the lives of Mozambican children.
Fifty percent of Mozambique’s total annual health expenditure is funded by external national and multilateral donors.
Consequently, a transformative quantum leap in terms of results and impact on health will only be possible if the strategic, technical and financial collaboration of external, national and multilateral donors not only holds steady but increases quite substantially in the coming years. The necessary investments in the top-priority strategies for the final battle against pneumonia will only be possible if there is strong political will and a solid global commitment to the SDGs and, more importantly, to the children of Mozambique.
* The author would like to thank Berta Briones for her help with updating some of the information in this text.