New Study Explores How the Malaria Parasite Responds to Artemisinin-Based Treatment in Infected Patients
Results indicate that in some cases the antimalarial increases the parasite's rate of sexual conversion and may thus attenuate the drug's effect in reducing parasite transmission
18.08.2022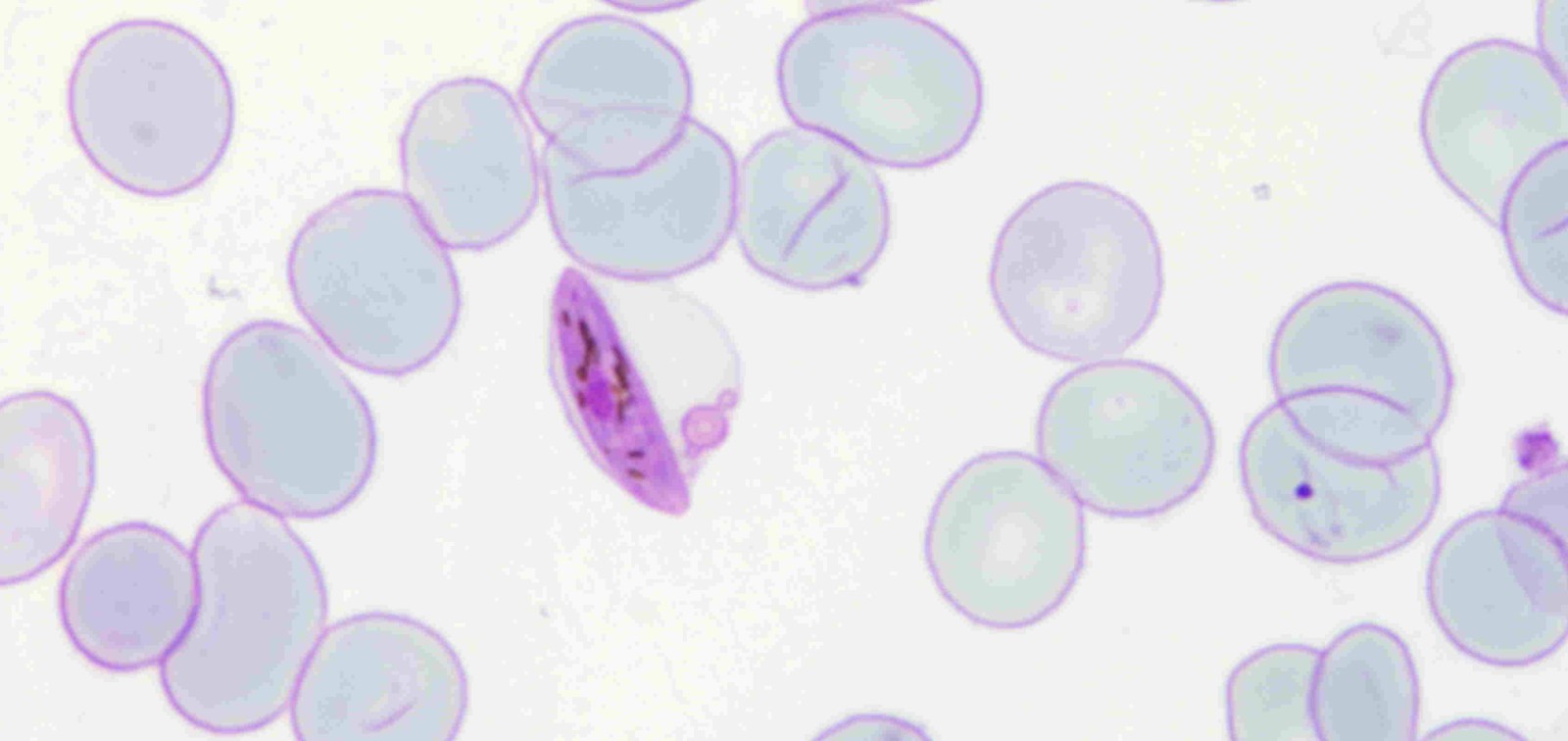
In most patients infected with P. falciparum, treatment with artemisinin increases the parasite's sexual conversion rate, which would attenuate the beneficial effect of the drug in reducing disease transmission. This is the main conclusion of a study led jointly by ITM in Belgium and ISGlobal, a centre supported by the "la Caixa" Foundation, and published in eBioMedicine.
The clinical symptoms of malaria result from the asexual reproduction of the parasite (P. falciparum) in the blood. But in each replicative cycle, a small fraction of parasites develop into the sexual form (gametocytes), which is the only form capable of infecting the mosquito and thus being transmitted to another person.
"We know that environmental conditions largely determine the proportion of parasites that convert into gametocytes, and thus the level of disease transmission," explains Alfred Cortés, ICREA researcher at ISGlobal, who has been studying the sexual conversion process for several years. In fact, his group had already shown that, in the laboratory, sexual conversion increases when the parasite is exposed to artemisinin, a first-line antimalarial drug.
In this study, Cortés and his team tested whether this effect of artemisinin is also observed in vivo - that is, in natural infections. To do so, they analysed blood samples from more than 100 malaria patients from Mozambique, Burkina Faso or Vietnam, taken before and at various intervals after administering the drug. "Thanks to the use of molecular markers of sexual conversion, we can distinguish between the effects of the drug on parasite viability and the effects on sexual conversion," explains Harvie Portugaliza, first author of the study.
The results show that, in most patients from Mozambique and Burkina Faso, artemisinin increased the expression of molecular markers of sexual conversion. This was not observed in samples from Vietnam, indicating that the effect of artemisinin on sexual conversion is complex, and also depends on other parasite or host factors. "Our analysis suggests that artemisinin resistance, which is common in Vietnam due to a mutation in a parasite gene, could be a factor in explaining the difference between the cohorts," explains Cortés, although he notes that further studies are needed to confirm this association and unravel other possible reasons.
The authors postulate that the effect of artemisinin in reducing disease transmission by reducing the number of viable parasites may be offset to some extent by an increase in the sexual conversion rate. This may be particularly relevant in individuals treated with suboptimal doses of the drug or in mass drug administration campaigns.
"Our study also validates a series of molecular markers that may be very useful for future studies on the impact of environmental factors on parasite sexual conversion and parasite transmission," adds Cortés.
Reference
Portugaliza HP, Natama HM, Guetens P et al. Plasmodium falciparum sexual conversion rates can be affected by artemisinin-based treatment in naturally infected malaria patients. eBioMedicine, 2022. doi: 101016/j.ebiom.2022.104198



