Unmasking the Hidden Burden of Tuberculosis in Mozambique
Using highly sensitive molecular techniques, a post-mortem analysis detects tuberculosis cases that would have otherwise been missed
01.08.2019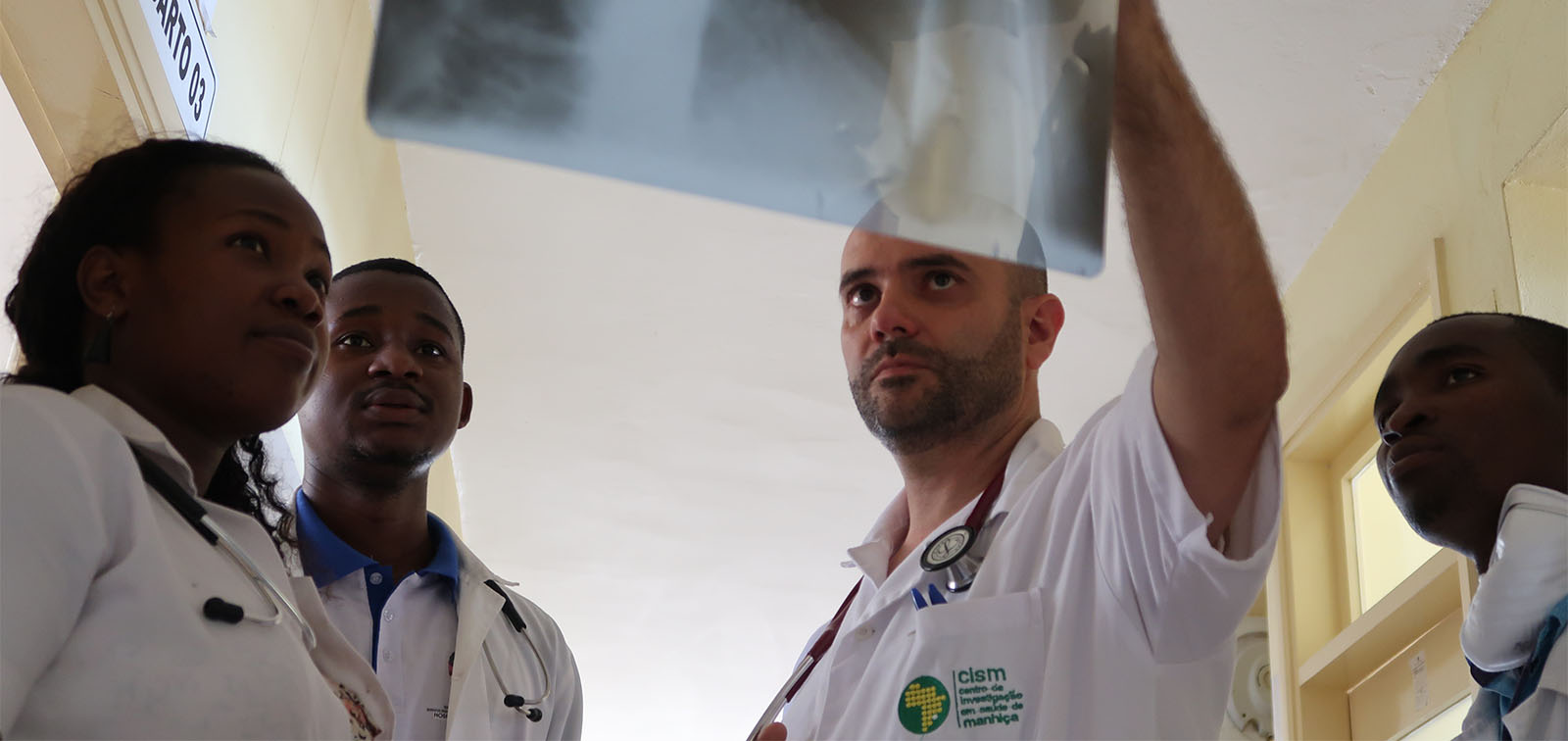
The real burden of tuberculosis (TB) is probably higher than estimated, according to a study on samples from autopsies performed in a Mozambican hospital. The study, led by the Barcelona Institute of Global Health (ISGlobal), an institution supported by ”la Caixa”, shows that highly sensible molecular techniques can detect cases that escape clinical diagnosis and even traditional post-mortem examination of organs and tissues.
TB is the leading infectious cause of disease globally and the most frequent cause of HIV-related deaths. In 2017, there were 10 million cases and 1 million TB deaths, according to WHO figures. But estimating the real burden of TB mortality is not easy, since clinical diagnosis or verbal autopsies are often unreliable.
Under the framework of CaDMIA, a project that seeks to validate the use of minimally invasive autopsies to determine causes of death and that is directed by Dr Jaume Ordi, Dr Clara Menéndez and Dr Quique Bassat, a team led by ISGlobal researcher Miguel Martinez performed a post-mortem study to evaluate the real TB burden in a hospital in Southern Mozambique, a region where the HIV and TB epidemics have devastating consequences. The research team analysed clinical data and samples from 223 complete autopsies performed on children, mothers and other adults. “The detailed histopathological and microbiological analysis we performed during the autopsies represents the most reliable way of identifying the cause of death and generating reliable information on the burden of TB,” says Miguel J. Martínez.
The results indicate that TB was the cause of death in 31 of the 223 cases; in 31 other cases disease signs were detected although it was not the cause of death. Most of these cases were incorrectly diagnosed by the clinician. In 18 additional cases, genetic material of the M. tuberculosis bacterium was detected, without any clinical or histological sign, which could reflect very early stages of the disease.
“This investigation is part of one of the largest autopsy studies conducted to date in sub-Saharan Africa,” says Alberto García-Basteiro, ISGlobal researcher and first author of the study, “and reveals the enormous burden of tuberculosis among children and adults that die in a reference hospital in Mozambique. Overall, 28% of patients had the disease at the time of death. The TB burden was even higher in HIV-positive adults (M. tuberculosis was detected in up to 51% of cases).
The results of the study, published in the European Respiratory Journal, also reveals the high number of cases that are missed by clinicians. “The routine use of these molecular techniques among patients in severe condition in high-burden TB countries could result in earlier detection of the disease and a better clinical management and prognosis of tuberculosis patients,” adds García-Basteiro.
Reference
Garcia-Basteiro AL, Hurtado JC, Castillo P, Fernandes F, Navarro M, Lovane L, Casas I, Quintó L, Jordao D, Ismail MR, Lorenzoni C, Carrilho C, Sanz A, Rakislova N, Mira A, Alvarez-Martínez MJ, Cossa A, Cobelens F, Mandomando I, Vila J, Bassat Q, Menendez C, Ordi J, Martínez MJ. Unmasking the hidden tuberculosis mortality burden in a large postmortem study in Maputo Central Hospital, Mozambique. Eur Respir J. 2019 Jul 25. pii: 1900312. doi: 10.1183/13993003.00312-2019. [Epub ahead of print] PubMed PMID: 31346005.



