WHO Recommends the First Malaria Vaccine for Children at Risk
ISGlobal, who has greatly contributed to the clinical development of the RTS,S/AS01 vaccine, joins the celebration of this historical recommendation which will help reinvigorate the fight against malaria
07.10.2021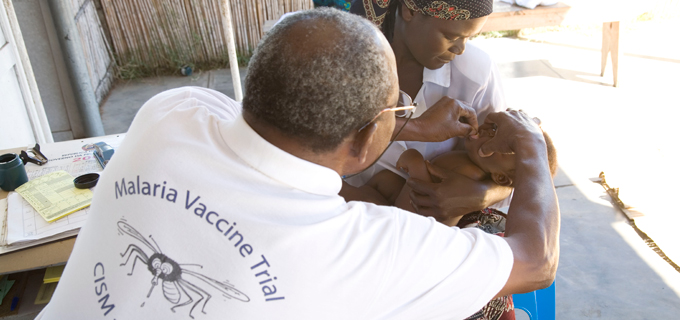
Yesterday, a historical milestone was reached in the fight against malaria. The World Health Organization (WHO) announced it is recommending widespread use of the first, long-awaited, malaria vaccine (RTS,S/AS01) among children in sub-Saharan Africa and in other regions with moderate to high transmission of P. falciparum malaria. The vaccine should be provided in a schedule of four doses in children five months of age or older. The recommendation, made by two WHO advisory bodies (one for immunisation and one for malaria) is based on the results from a large-scale pilot programme in Ghana, Kenya and Malawi that has reached more than 800,000 children since 2019.
The pilot trial showed that the vaccine is feasible to deliver through routine immunization systems, even in the context of the COVID-19 pandemic. It showed that the vaccine also benefits children who are not sleeping under a bednet, so that over 90% of children benefited from at least one preventive intervention (bednets or vaccine). A significant reduction (30%) in deadly severe malaria was observed, even in areas where bednets are used and there is good access to diagnosis and treatment. The vaccine showed a strong safety profile (over 2.3M doses have been administered), and had no negative impact on the uptake of bednets or other childhood vaccinations.
“This is a historical recommendation, and I would like to congratulate all who have contributed to this point, starting with parents and children who participated in the trials, participating research institutions across Africa, MVI PATH, philanthropic funding from BMGF, and most importantly, leadership in the three participating countries - Ghana, Malawi, Kenya”, said Regina Rabinovich, director of the Malaria Elimination Initiative at ISGlobal, and founding director of the Malaria Vaccine Initiative at PATH, which supported the development of RTS,S/AS01 since its early phases.
“ISGlobal contributed with the design and implementation of the innovative phase 2b trial, which set the stage for subsequent work” adds Rabinovich. In fact, the first proof of concept studies that confirmed security and efficacy of the vaccine in babies and small children were carried out in 2004 in Mozambique, as a collaboration between ISGlobal (formerly the Barcelona Center for International Health) and the Manhiça Health Research Centre (CISM), under the leadership of Pedro Alonso, ISGlobal founder and current director of the WHO Global Malaria Program. These results set the basis for a multicentric phase 3 trial across 11 African countries, which in turn led to a positive opinion by the European Medicine Agency and a recommendation by the WHO to perform the above-mentioned pilot trial in Ghana, Kenya and Malawi, launched in 2019.
In addition to the clinical development of the vaccine, ISGlobal, an institution supported by “la Caixa” Foundation, has pursued important work in characterising the immune responses induced by RTS,S/AS01. For ISGlobal researcher Carlota Dobaño, who has led many of these studies, it is a privilege to witness a positive recommendation for the first malaria vaccine for African children. “The pilot study has further confirmed that RTS,S/AS01 vaccination is feasible, safe and has a significant impact on preventing malaria hospitalizations, despite its partial and relatively short efficacy,” she says. “This milestone is a first step towards preventing this deadly disease while we continue investigating the immune mechanisms and factors underlying protection, and work towards developing more efficacious second-generation vaccines."
Quique Bassat, director of the Malaria Programme at ISGlobal and who was involved in the early trials in Manhiça as a young paediatrician, adds: “I'm personally overjoyed to see that the vaccine candidate to which we have devoted so many years of hard work in its clinical development is now a reality, and will contribute to saving the lives of thousands of children each year. This first-generation malaria vaccine is a major breakthrough in global public health.” For the paediatrician, who has seen first-hand the terrible consequences of this disease on child health, there is no greater public health intervention than that aimed at reducing child mortality. “Having a malaria vaccine deployed in Sub-Saharan Africa will substantially improve child survival, and the lives and health of so many people affected by malaria every year,” he adds.
For the global health community, this recommendation is particularly relevant at a moment in which progress against malaria is stalling. The vaccine represents an additional tool that will help reinvigorate the fight against such a devastating disease.



